Testosterone Replacement Therapy (TRT) is a medical treatment used to restore testosterone levels in men who have been diagnosed with low testosterone. When levels fall below a healthy range, it can affect energy, mood, sexual health, body composition, and overall wellbeing.
In the UK, TRT is available through both the NHS and private clinics. Access to treatment typically begins with proper blood testing and medical evaluation to confirm whether testosterone deficiency is present and whether treatment is appropriate.
This guide provides an overview of how TRT works in the UK, including symptoms of low testosterone, how blood testing and diagnosis work, treatment options available to patients, and how monitoring is carried out once treatment begins.
Testosterone Replacement Therapy increases testosterone levels in men whose bodies are not producing sufficient amounts of the hormone naturally.
The aim of treatment is to restore testosterone to a healthy physiological range and reduce symptoms associated with deficiency. Depending on the patient and clinical recommendation, testosterone may be prescribed in several formats including injections, topical treatments, or oral medications.
Testosterone plays a major role in male health and influences a wide range of functions including:
When testosterone levels drop significantly below an optimal range, these systems can begin to decline.
Read more about TRT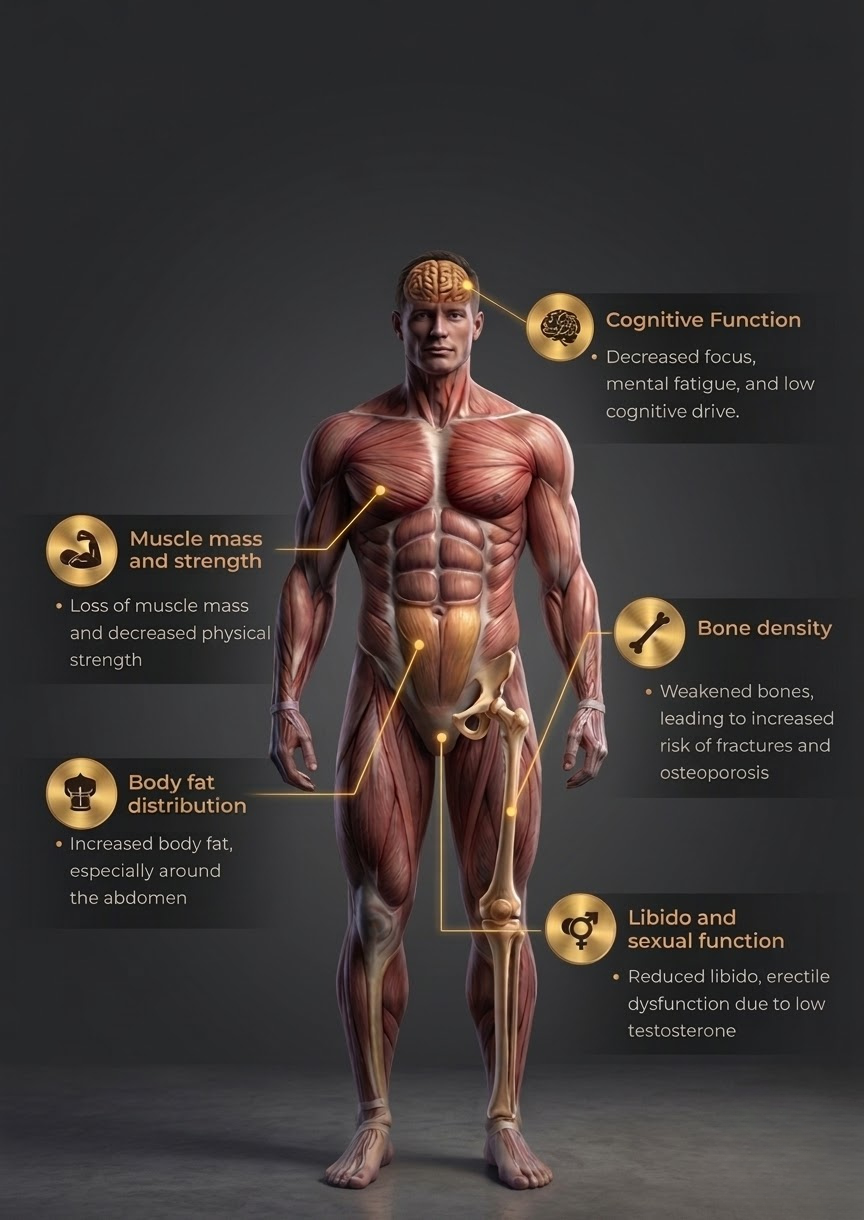
Testosterone levels typically peak during early adulthood and gradually decline with age. Research suggests that levels decrease by around 1–2% per year from the age of around 30.
While this gradual reduction is considered normal, some men experience a sharper decline or develop hormone deficiencies earlier in life. When this reduction is significant and confirmed through blood testing, it may be diagnosed as testosterone deficiency.
Low testosterone is relatively common, particularly in men over 40, although it can affect younger men as well.
Read more about natural testosterone decline
Testosterone affects multiple biological systems, which means low levels can produce a wide range of symptoms. These symptoms often develop gradually and may be mistaken for stress, ageing, or lifestyle factors.
Common symptoms associated with low testosterone include:
Many of these symptoms overlap with other health conditions, which is why proper blood testing and medical evaluation are required before diagnosing testosterone deficiency.
Read more about low testosterone symptomsTestosterone is a powerful hormone and treatment should only begin following appropriate medical assessment.
There are several reasons why a professional diagnosis is important.
Low testosterone can sometimes be the result of another medical condition, hormonal imbalance, medication, or lifestyle factor. Identifying the root cause is an important step before considering hormone therapy.
In the UK, testosterone is classified as a controlled substance under the Misuse of Drugs regulations. Personal possession of testosterone is legal. However, it is illegal to supply, sell, or distribute testosterone without the appropriate prescription and medical authorisation.
Because testosterone is a powerful hormone that affects multiple systems in the body, treatment should still only be undertaken under medical supervision. Proper testing and guidance from a qualified healthcare professional helps ensure treatment is safe, appropriate, and tailored to the individual.
Even when testosterone levels are low, treatment may not always be the best course of action. Doctors review blood results alongside medical history, current medications, lifestyle factors, and fertility considerations before recommending therapy.
Symptoms commonly associated with low testosterone may also be linked to sleep disorders, thyroid problems, mental health conditions, or metabolic issues. Medical testing helps rule out other explanations before treatment is considered.
Blood testing is the first step in determining whether testosterone levels are within a healthy range.
Because testosterone levels fluctuate throughout the day, tests are typically carried out in the morning, usually between 7am and 11am when levels are naturally highest.
Testing may take place in several different settings depending on the route a patient takes.
If you visit your GP, they may be willing to arrange blood testing to investigate symptoms. However, not all GP practices routinely test for a full range of hormone markers unless there is strong clinical suspicion.
Private clinics frequently arrange blood testing through partnered laboratories or national providers with pharmacy collection locations across the UK. Some clinics also operate their own physical testing facilities.
Home finger-prick blood tests are sometimes offered by online services. These tests can provide a general overview of hormone levels but are usually considered insufficient for diagnosing testosterone deficiency on their own. A full venous blood test is typically required before treatment is prescribed.
Doctors review a broad panel of biomarkers when assessing hormone health. A comprehensive assessment before treatment should ideally include markers such as:
This type of testing provides a full picture of hormonal balance and overall health before testosterone therapy is considered.
Read more about blood testing and diagnosisTestosterone Replacement Therapy can be prescribed through the NHS for patients who meet diagnostic criteria.
For most men, the first step is visiting their GP to discuss symptoms or concerns about hormone levels. If low testosterone is suspected, the GP may arrange blood tests and investigate potential causes.
If results confirm testosterone deficiency, the patient may be referred to an endocrinologist who specialises in hormone-related conditions.
However, experiences with NHS assessment can vary significantly.
Some men report being dismissed despite presenting symptoms consistent with testosterone deficiency, or having testosterone levels within ranges considered treatable under guidelines set by organisations such as the British Society for Sexual Medicine (BSSM) and the International Society for Sexual Medicine (ISSM).
Access to specialist assessment can also involve long waiting times depending on location and referral pathways.
Because of these factors, some men choose to explore private clinics for testing and treatment.
Read more about NHS TRTPrivate clinics offer an alternative route for men seeking testosterone testing and treatment.
Many of these clinics specialise in hormone health and men’s health, allowing them to focus more heavily on hormone-related conditions.
The process typically includes comprehensive blood testing, consultation with a doctor experienced in TRT, confirmatory testing where required, and development of a personalised treatment plan.
Private providers may also analyse additional hormone markers and look more closely at the balance between different types of testosterone within the body.
Private treatment generally involves higher costs than NHS care. Pricing varies depending on the clinic, medication type, monitoring schedule, and consultation frequency.
If testing confirms testosterone deficiency and treatment is recommended, several therapy formats may be considered.
Injectable testosterone is one of the most common forms of treatment. Injections deliver testosterone directly into the bloodstream and are administered at regular intervals depending on the medication used.
Topical testosterone can be applied daily to the skin.
Within the NHS, testosterone gels are commonly prescribed. In private practice, gels are used less frequently, while testosterone creams have become increasingly popular as some patients report more stable results and easier dose adjustments.
Some clinics prescribe oral testosterone formulations such as testosterone undecanoate.
Other medications, such as clomiphene (often referred to as Clomid), may also be used in certain situations to stimulate natural testosterone production. However, responses can vary and some patients report unwanted side effects, which means these treatments may not be suitable for everyone.
The most appropriate treatment format depends on the patient’s blood results, medical history, symptoms, and response to therapy.
Read more about TRT treatment optionsRegular monitoring is an essential part of safe testosterone therapy.
Follow-up blood testing allows doctors to track hormone levels, ensure treatment is working effectively, and identify any potential issues early.
Monitoring typically includes reviewing many of the same biomarkers assessed during the initial diagnosis.
Regular testing allows doctors to adjust dosage if necessary and ensure testosterone levels remain within a safe and effective range.
Read more about TRT monitoringTestosterone Replacement Therapy can significantly improve symptoms for men who have clinically low testosterone levels. However, treatment should always begin with proper testing and professional medical evaluation.
In the UK, both NHS services and private clinics provide pathways for diagnosis and treatment. Understanding how the process works—from recognising symptoms to blood testing, treatment selection, and ongoing monitoring—helps patients make informed decisions about their health.
For anyone experiencing symptoms associated with low testosterone, arranging proper blood testing and speaking with a qualified medical professional is the most reliable first step.
Read more about starting TRT in the UK
TRT is used to restore testosterone levels in men who have been diagnosed with testosterone deficiency and are experiencing symptoms associated with low testosterone.
Symptoms alone are not enough for diagnosis. Proper blood testing, symptom review, and medical evaluation are required before testosterone deficiency can be confirmed.
Yes. TRT can be prescribed through the NHS for patients who meet diagnostic criteria, although access, testing thresholds, and referral experiences may vary.
A proper assessment may include Total Testosterone, Free Testosterone, SHBG, Albumin, Oestradiol, Prolactin, LH, FSH, thyroid markers, PSA, liver function, kidney function, full blood count, ferritin, lipid profile, and HbA1c.
Depending on the patient and clinical recommendation, treatment options may include testosterone injections, topical gels or creams, and in some cases oral treatments or other medications.
Yes. Regular follow-up blood testing and medical review are essential to ensure treatment is working effectively and that testosterone levels remain within a safe and appropriate range.
Fill out the form below and we will get back to you within the next 24
hours to complete the order, and then you’re all set to get started!